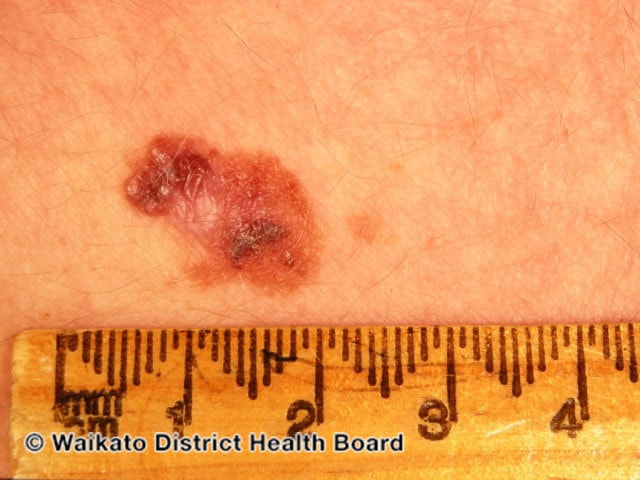
Melanoma Basics
Melanoma (also known as malignant melanoma) is a serious form of skin cancer that begins in melanocytes, the pigment-producing cells in our outermost layer of skin. Melanoma is less common than both basal cell carcinoma and squamous cell carcinoma, but more dangerous due to its ability to spread to other organs more rapidly if not treated at an early stage. Due to this fact, early diagnosis and treatment of melanoma is crucial.
More than 1 million people are living with melanoma, and one person dies of the disease every hour. However, the estimated five-year survival rate for U.S. patients whose melanoma is detected early is about 98 percent. The survival rate drops to 63 percent if the disease has reached the organs and 20 percent if it has spread to the lymph nodes.
Melanoma Risk Factors
Risk factors for melanoma include:
- Already diagnosed atypical moles
- Unprotected or excessive UV exposure, either from the sun or from indoor tanning
- A weakened immune system due to a medical condition or medications
- Many moles or large moles: The more moles you have, the higher your risk. Having moles larger than the tip of a pencil also puts you at increased risk.
- Fair skin
- Family history and genetics
Melanoma Prevention & Detection
We recommend you remain vigilant to both prevent and detect melanoma in its earliest and most easily treatable stages.
Preventative measures include:
- Stay out of the sun, especially between peak sunlight hours between 10 a.m. and 4 p.m.
- Cover up with clothing, including a broad-brimmed hat and UV-blocking sunglasses
- Apply broad-spectrum (UVA/UVB) sunscreen with an SPF of 35 or higher to your entire body 30 minutes before going outside. For extended outdoor activity, use a water-resistant, broad-spectrum sunscreen with an SPF of 35 or higher. Reapply every two hours or immediately after swimming or heavy sweating.
- Do not burn, tan or use tanning booths
- Keep newborns out of the sun. Use sun protection on babies age 6 months and older.
Melanoma can appear as an existing mole or as a new lesion. When it begins as a mole that is already on the skin, it tends to grow on the surface of the skin for some time before penetrating more deeply. While melanoma can be found anywhere on the body, it is most likely to appear on the torso in men, on the legs in women and the upper back in both men and women.
If you have any of the risk factors listed above, we recommend performing a monthly skin self-exam to aid in the early detection of melanoma. You can get a free self-exam worksheet here.
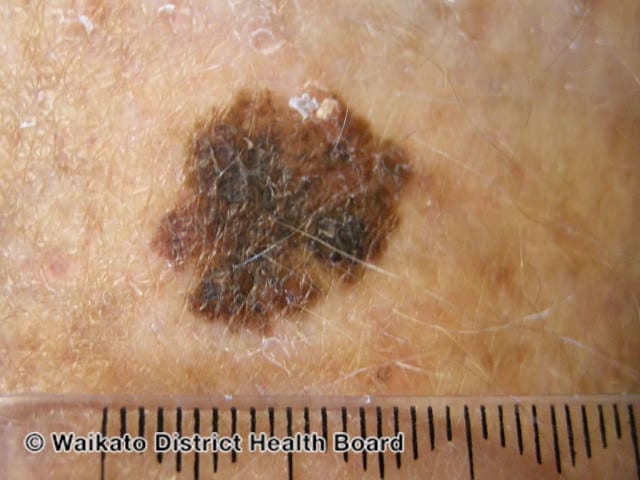
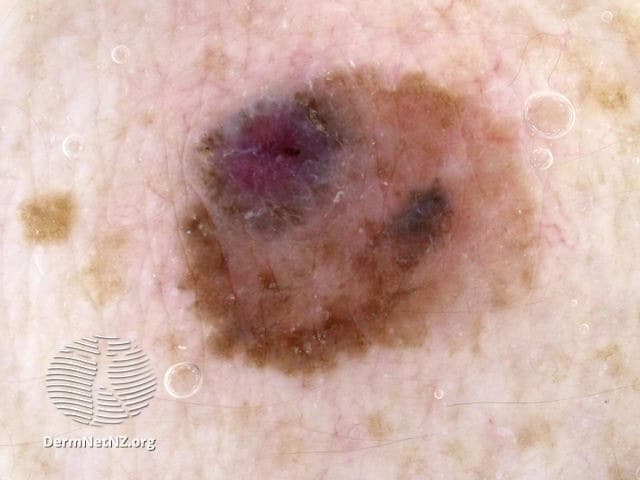
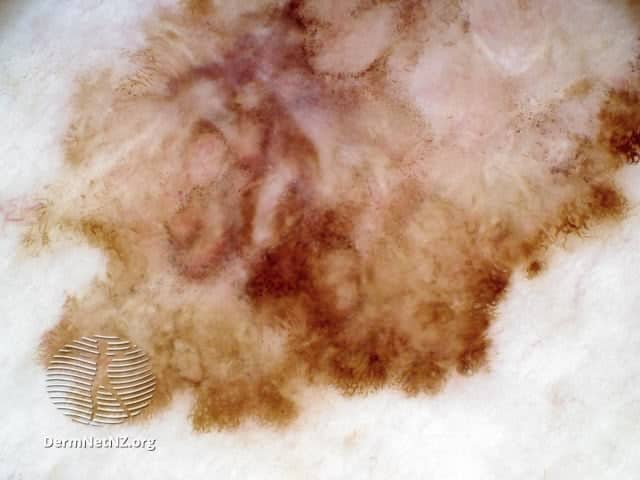
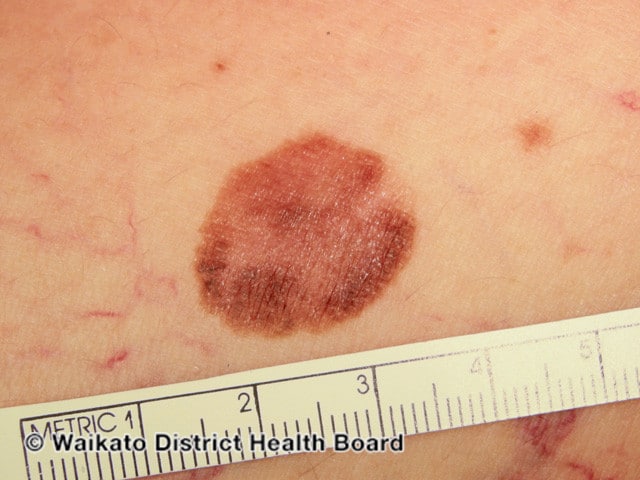
When you perform your self-exam, check all your spots for the ABCDE’s of melanoma:
- A. Asymmetric: If you could fold the spot in half, the sides would not match.
- B. Uneven Border: Moles tend to have a smooth, even border. By contrast, melanoma tends to have a jagged (or uneven) border.
- C. Color: Is varied from one area to another; has shades of tan, brown or black, or is sometimes white, red or blue.
- D. Diameter: Melanomas are usually greater than 6mm (the size of a pencil eraser) when diagnosed, but they can be smaller.
- E. Evolving: A mole or skin lesion that looks different from the rest or is changing in size, shape or color.
In addition to regular self-exams, schedule a skin cancer screening annually to have us perform a professional full-body cancer screening. Make your appointment now.
Melanoma Diagnosis
When you visit our office because you’ve noticed a suspicious-looking spot on your skin, your dermatologist will first perform a physical exam and gather information about your health history. Then, depending upon this evaluation, your dermatologist may remove a portion of the lesion if he or she suspects the potential for skin cancer. This is called a skin biopsy. A biopsy is essential because it’s the only way to determine the presence of skin cancer with 100 percent certainty.
A pathologist will examine the skin your dermatologist has removed under a microscope, looking for skin cancer cells. The pathologist will then provide a biopsy report to your dermatologist to direct our next steps of treatment
It can take one to two weeks for your dermatologist to receive and review your biopsy report. These results will guide further followup or treatment. If a diagnosis of skin cancer is confirmed, we will help you determine the most appropriate course of care.
Melanoma Treatment
Your biopsy will determine the subtype and stage of your melanoma, which will guide our treatment. In its early stages, melanoma can be treated with surgical excision with microscopic margin control. This multi-day step by step surgical treatment is similar to Mohs surgery where the entire margin is carefully examined, but the tissue is processed overnight for the highest identification of the melanoma cells. This will give the highest cure rate, especially on the head and neck and other areas of extensive sun damage.
If your melanoma is more invasive, further diagnostic tests will be necessary, such as lymph node biopsy or CT/PET scans to help determine if the cancer has spread beyond the skin. If these confirm that your melanoma has spread, more aggressive surgeries and systemic treatments may be necessary.