Basal cell carcinoma (BCC) is the most common form of skin cancer. An estimated 4.3 million cases of basal cell carcinoma are diagnosed in the U.S. each year.
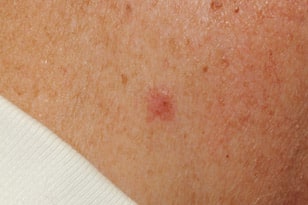
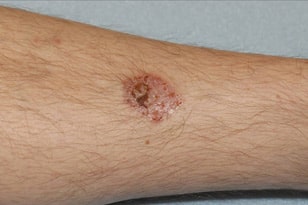
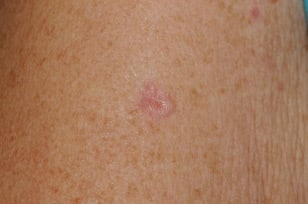
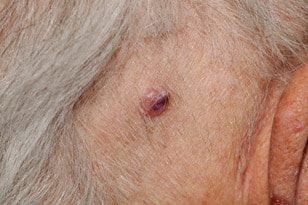
Basal cell carcinoma starts in the top layer of skin (the epidermis) and is often related to sun exposure or indoor tanning. It can appear to be a pink and/or scaly patch of skin or as a flesh-colored pearl-like bump on the skin. It typically develops in people with fair skin, although it can also affect people with darker skin. Basal cell carcinoma are commonly located on the head, neck and arms, but they can form anywhere on the body, including the chest, abdomen and legs.
Basal cell carcinoma can be caused by periods of intense sun exposure as well as cumulative sun exposure. Fair skin and skin damaged by burns, serious wounds, inflammatory skin conditions, and exposure to radiation and harmful chemicals also make you vulnerable.
Signs of a Basal Cell Carcinoma
- A red area of dry skin that does not heal
- A mole-like, pearly bump that is white, pink, red, tan, brown, or black
- A persistent pimple
- A sore that doesn’t heal
- A waxy white, yellow, or skin-colored scar with irregular borders
- Shiny pink or red growths that look like sores and bleed easily, often with scaly spots
- A hard, flat or sunken growth, usually white or yellow
How to Prevent Basal Cell Carcinoma
Ultraviolet light is the most preventable risk factor for all types of skin cancer, including basal cell carcinoma. Protect your skin from UVA/UVB rays anytime you’re outdoors by:
- Apply sunscreen
Be sure to use a broad-spectrum sunscreen of SPF 30 or higher
- Re-apply sunscreen
A good rule of thumb is to re-apply suncreen every two hours or after swimming or sweating
- Be smart about being in the sun
Wear a wide-brimmed hat and sun-protective clothing, and plan to enjoy the outdoors during non-peak sunlight hours
- Avoid tanning beds
Avoid tanning beds, which can cause premature aging and skin cancer
Basal Cell Carcinoma Diagnosis
Early diagnosis and treatment for basal cell carcinoma is important because this type of skin cancer can invade the surrounding tissue and grow into nerves, muscle or cartilage, causing damage and disfigurement. However, when caught early, basal cell carcinoma is highly treatable.
When you visit our office because you’ve noticed a suspicious-looking spot on your skin, your dermatologist will first perform a physical exam and gather information about your health history. Then, depending upon this evaluation, your dermatologist may remove a portion of the lesion if he or she suspects the potential for skin cancer. This is called a skin biopsy. A biopsy is essential because it’s the only way to determine the presence of skin cancer with 100 percent certainty.
A pathologist will examine the skin your dermatologist has removed under a microscope, looking for skin cancer cells. The pathologist will then provide a biopsy report to your dermatologist to direct our next steps of treatment
It can take one to two weeks for your dermatologist to receive and review your biopsy report. These results will guide further followup or treatment. If a diagnosis of skin cancer is confirmed, we will help you determine the most appropriate course of care.
Basal Cell Carcinoma Treatment
The preferred treatment for your basal cell carcinoma depends on its size and location. Some low-risk forms of basal cell carcinoma may be treated with a procedure called curettage. Topical chemotherapy creams can also sometimes be appropriate for BCC. Surgical excision is frequently used for basal cell carcinoma less amenable to curettage or topical treatments. Occasionally, radiation or systemic medications are recommended.
Mohs Micrographic Surgery is an advanced treatment for basal cell carcinoma. It has the highest cure rate and also spares the most surrounding skin, offering you the best cosmetic and functional outcome. Mohs surgery is often the treatment of choice for higher-risk skin cancers or skin cancers in areas where there is not as much surrounding skin or tissue, such as the face, ears, scalp and hands. For full details about this procedure, please visit our Mohs Surgery information page.